In this series of articles, two patients John and Jill (aliases) will share their personal patient journey with us. We are very thankful for sharing their personal experiences and shed some light on the broad spectrum of kidney disease. This part focuses on the period after the diagnosis when the disease progression should be slowed down, e.g. through dialysis or adapted nutrition.
Furthermore, thanks to the contributing experts from our partners for their input for this article: Dr. Marcel Naik (Charité), Dr. Mozhgan Bayat (HPI), Dr. Matthieu-P. Schapranow (HPI). Images by Elf moondance, Mohamed Hassan and John.
Progression of kidney disease and impact of medications
In part I of the patient journey, we have learnt about the stages of chronic kidney disease (CKD) defined based on the patient’s estimated glomerular filtration rate (eGFR). The main focus of CKD therapy is to slow down disease progression to delay the start of dialysis and the complete loss of function. Therefore, the nephrologist aims to reduce impact of existing comorbidities, e.g. high blood pressure, diabetes mellitus, through optimized personal diet.
For stages I-III, changes of diet and lifestyle might be already very beneficial to compensate for reduced kidney function, e.g. less water, quit smoking, more walking. Nephrologists focus on teaching the patients to maintain a healthy lifestyle. The nephrologist will also review existing medical intake, e.g. due to comorbidities, because some of them, e.g. pain killers, might contribute to reduced kidney function. From stage IV on, the patient’s nephrologist will decide on the start of dialysis to assist regular cleaning of the blood. In stage V, when the kidney completely failed, the patient needs a renal replacement therapy such as constant dialysis and kidney transplantation. Even when a patient is on a waiting list for a donor organ, dialysis is necessary to clean the blood and remove extra water from the body.
Special diets recommendations for kidney patients and medications restriction
One of the kidney tasks is to balance electrolytes, e.g. potassium and phosphate. Therefore, it is crucial for CKD patients to reduce the intake of such trace elements to reduce additional stress on the organs. A high potassium intake while having a reduced kidney function might contribute to additional kidney damage and systemic side effects.
Injured kidneys cannot clear potassium very well. When the potassium level gets too high, it can lead to an irregular heartbeat – arrhythmia –, which may lead to death if untreated. Fruits such as bananas and vegetables such as potatoes are rich sources of potassium. Phosphate is used to increase the shelf life of food, but it is also contained in dairy and many meat products. As phosphate binds together with calcium, it becomes more difficult to extract it from the blood with dialysis. CKD patients can suffer from phosphate excess, which is one major factor for arteriosclerosis and mortality from cardiovascular causes. CKD patients should try sports regularly in their daily life. Furthermore, it is important to eat healthy food and be aware of the consumption of potassium and phosphate in their daily food and try to reduce it to a minimum level.
John: “When it comes to the potassium and phosphate diet that is important for a dialysis patient. As a dialysis patient, I always pay attention to my diet. Over the years I developed a good feeling about consumption of potassium and phosphate in my diet. Sometimes I allow myself a portion of French fries. My dialysis nurses and doctors never condemned me or even complained about consumption of potassium and phosphate, and sometimes if I had totally overdone it, it was brought to my attention immediately.”
Certain drugs can cause further damage to a damaged kidney, e.g. pain killers (ibuprofen, indomethacin, piroxicam or celecoxib), antibiotics (gentamicin, penicillins, ciprofloxacin, rifampicin, tetracyclines), immunosuppressants (cyclosporine or tacrolimus), and antivirals (aciclovir, interferon). In most cases, an appropriate dose assessment coordinated by the nephrologist is necessary. From a certain degree of kidney impairment, certain drugs are prohibited (metformin), because life-threatening side effects can occur due to the reduced ability to excrete the drugs.
Dialysis as a renal replacement therapy
There are two modes of dialysis: haemodialysis and peritoneal dialysis. Dialysis helps to restore levels of electrolytes such as potassium, phosphate, etc. Another important function of dialysis is to extract water from the patient to re-balance fluid levels. By extracting accumulated water through dialysis from the body, the blood pressure of the patient can be controlled.
There are five indicators to start dialysis:
- Severe acidosis (low blood pH) that impede normal metabolism,
- Electrolyte disturbances (hyperkalemia) that may lead to severe cardiac events, e.g. cardiac arrhythmia or arrest,
- Unintended intoxication due to intake of certain substances (lithium, antidepressants, methanol),
- Uremia (accumulation of toxic substances in the blood)
- High fluid retention in the body leading to breathing problems for the patient.
Haemodialysis
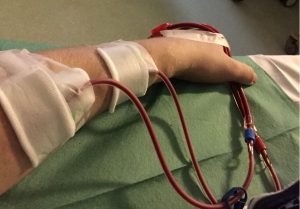
Jane has received haemodialysis because of a fluid accumulation led to breathing problems in her AKD case. Therefore, catheters were placed into a blood vein. One cather for taking out the blood of the vein injecting it into the haemodialysis machine and one that brings back the blood from the machine to the patient’s blood system. The haemodialysis machine is equipped with safety installations, which stops the operation without harming the patient. Examples are: air traps, pressure measurements, and blood loss detectors. The main component of the haemodialysis machine is the dialyzer, in which blood and the dialysis fluid are separated only through a very thin semipermeable membrane that allows the exchange of low molecular weight substances and thus cleans the blood.
Jane was diagnosed with AKD: “Up until that point in my life I had never really thought about my kidneys.They had never caused any problems and worked just as well as the other organs in my body. Suddenly, I found myself in a hospital bed attached to a lot of machines while digesting a lot of medical information on the state of my body. High blood pressure, high pulse, water retention, reduced lung functioning, all these things were completely new to me and difficult to understand. It was only after a few days when I realized that one of the machines I was attached to was actually a haemodialysis machine.”
The haemodialysis machine requires a minimum blood flow of 100ml/min. The patient’s blood system contains approx. five to six liters of blood, whilst about half a liter is always in the haemodialysis machine. Nowadays, haemodialysis machines compared to peritoneal dialysis are more precise for regulating detoxification and fluid balance.
In John’s case, haemodialysis was permanently necessary. Therefore, a shunt that runs under the skin before entering the blood vessel was replacing the catheter to prevent infections, which could be threatening.
John was diagnosed with CKD: “In autumn 1989, my kidney had stopped working and I got dialysis for the first time at the age of 13. Together with nurses and doctors at the dialysis center, we decided on the amount of water withdrawal and heparin dose. My biggest problem has always been keeping the appropriate fluid level. There were days and nights when I cried in desperation as I knew that I had too much fluid intake, but still felt thirsty. Sometimes, I arrived at the dialysis center with six liters of water in my body after a weekend. Because of all the water in my body. The more water had to be drawn, the worse I felt after dialysis.”
Peritoneal dialysis
An alternative mode of dialysis is the peritoneal dialysis. A catheter is placed with a small operation into the abdominal cavity. The abdominal cavity serves as a container for the dialysis fluid. The surface lining (peritoneum) of the guts is used as a dialysis membrane and thus waste products are cleared replacing the dialysis fluid in regular intervals. Certain surgeries in the abdomen might make a patient ineligible for peritoneal dialysis.
The big advantage of peritoneal dialysis compared to haemodialysis is that the patient can do it at home without the need for medical assistance. However, the risk for life-threatening infections from peritonitis are comparable high, that is a major disadvantage for this type of dialysis. Furthermore, after five years half of the patients need to convert to haemodialysis as the characteristics of the peritoneum have changed.
The NephroCAGE consortium
The German Canadian consortium NephroCAGE combines medical and scientific-technical expertise from Germany and Canada. We jointly create a decentralized clinical prediction model that tests the added value of the latest artificial intelligence (AI) techniques on kidney transplantation patients in different transplant centers within Germany and Canada. Our clinical prediction models aim to support nephrologists in identifying post-transplant risks, e.g. graft loss. Amongst others, we incorporate duration and type of dialysis before kidney transplantation as important factors for graft function prediction in our clinical prediction models.





Comments are closed